The Prescription Transparency Gap: Why Many Employees Miss Out on Savings
- Buzz Health Research Team

- Mar 25
- 5 min read

Prescription drug costs are one of the biggest financial stressors facing American workers today, and millions are missing out on savings tools that could help. Buzz Health surveyed 1,007 full-time employees and 250 healthcare decision-makers to uncover how prescription affordability information is being shared in the workplace.
What we found was a striking disconnect between what employees experience and what their employers believe or communicate. This research breaks down where the gaps are, who feels them most, and what it would take to close them.
Key Takeaways
2 in 3 employees (67%) said their employer has never informed them about tools or programs to help reduce prescription drug costs.
Over 1 in 4 healthcare decision-makers (27%) admitted their company's health plan doesn't do enough to protect employees from high prescription drug costs.
Over 2 in 5 full-time employees (43%) made at least one health or financial sacrifice in the past year because a prescription was too expensive.
The most common sacrifices employees made were delaying filling a prescription until they could afford it (17%), using a credit card and carrying a balance (17%), and cutting back on groceries or food spending (12%).
Roughly 1 in 4 healthcare decision-makers (26%) said prescription affordability is "not a current organizational priority."
The Prescription Savings Tools Not Being Shared
For many employees, getting help with prescription costs had less to do with whether savings tools existed and more to do with whether anyone bothered to explain them. That communication gap left many workers on their own to figure things out before costs became a real problem.

Two in three employees (67%) said their employer had never informed them about tools or programs that could lower prescription drug costs. Meanwhile, only 42% of healthcare decision-makers said they hadn't communicated these tools, meaning what employers thought they shared didn't always match what employees actually heard.
That perception gap extended to costs as well, with decision-makers estimating employees paid a median of $100 per month for a brand-name prescription while employees reported a median of $30.
The communication drop-off also showed up across every type of savings tool:
Prescription discount cards: 65% of healthcare decision-makers were aware of them, but only 32% shared them with employees.
Manufacturer copay cards: 34% were aware, but only 17% communicated them.
State pharmaceutical assistance programs: 25% were aware of them, but only 8% shared them.
Even among employees who found and used a prescription discount program, only 10% heard about it from their employer. Most discovered it through a doctor or pharmacist (39%) or through an internet search (27%).
The Price Employees Pay
When prescriptions became too expensive, employees didn't just feel it at the pharmacy counter. The impact spilled over into their health decisions, finances, and everyday routines.
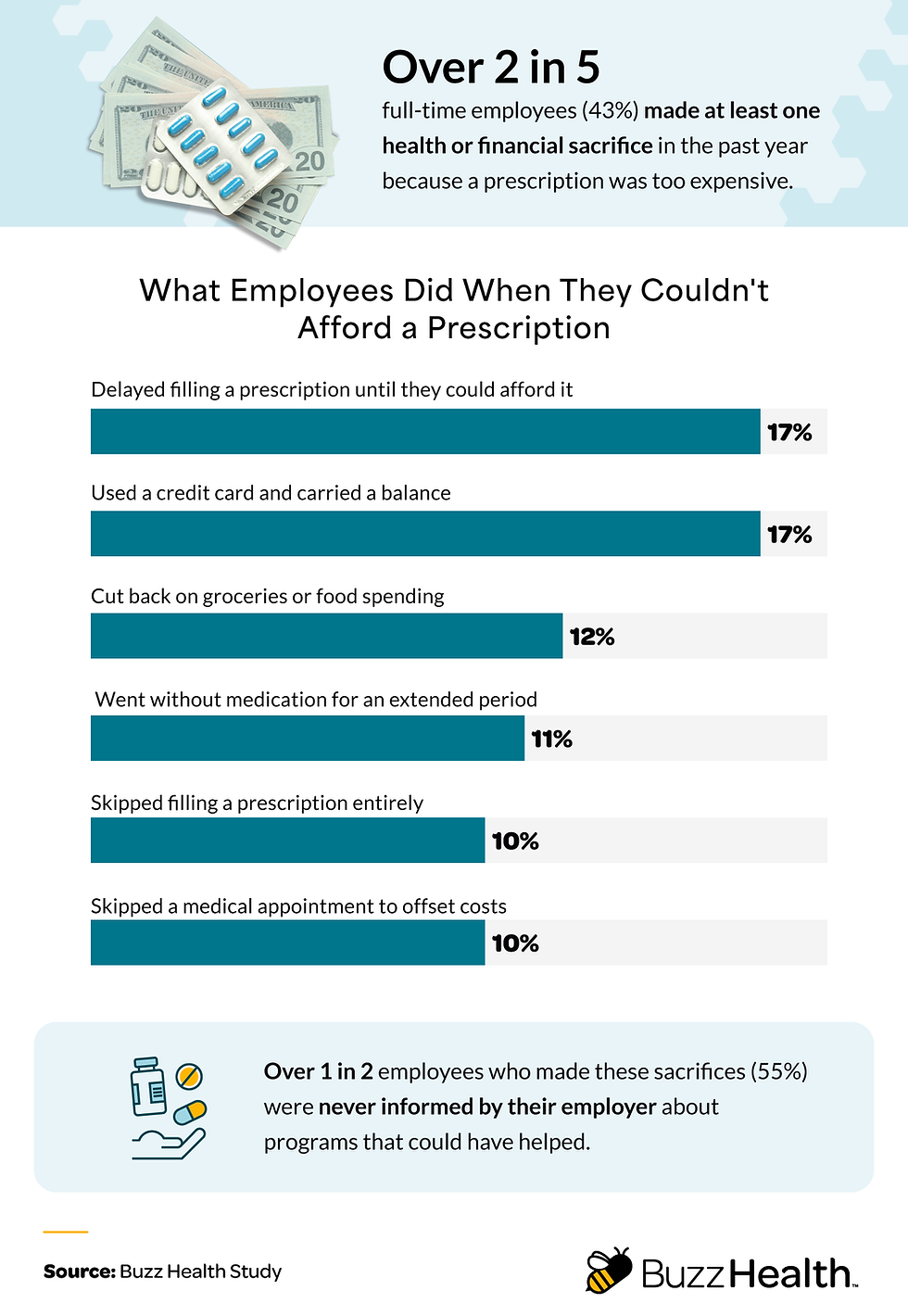
Over two in five full-time employees (43%) said they made at least one health or financial sacrifice in the past year because a prescription was too expensive. The most common tradeoffs included:
Delaying filling a prescription until they could afford it (17%)
Using a credit card and carrying a balance (17%)
Cutting back on groceries or food spending (12%)
Going without medication for an extended period (11%)
Skipping filling a prescription entirely (10%)
The strain reached beyond prescriptions alone. Another 10% skipped a medical appointment to offset costs. And more than half of employees who made these sacrifices (55%) said their employer had never informed them about programs that could have helped.
Some groups felt the burden more sharply than others. Over half of workers earning under $50K (52%) made at least one health or financial sacrifice, compared to only 26% of those earning $150K or more. Women were also more likely than men to report making at least one sacrifice (48% vs. 37%).
Younger and lower-income workers faced distinct pressures, too. Gen Z employees were the most likely to skip filling a prescription entirely, at 18%, double the rate reported by millennials and Gen X workers (both at 9%). Workers earning under $50K were also more likely to cut back on groceries (17%) compared to those earning $75K to $99K (8%).
The Inaction Gap
Prescription affordability sits in an uneasy place for many organizations. Employees feel the impact, but many workplaces still haven't treated it as a real priority.

Among employees earning under $50,000, 15% said they wanted to speak to HR about prescription costs but never did, and another 11% said they spoke to HR but didn't receive help. Prescription affordability also colored employees' overall view of their benefits, with 49% saying it significantly shaped their opinion of their benefits package.
Overall, 21% of employees rated their employer's prescription drug cost support as poor or worse, and just 7% rated it as excellent. Women were more likely than men to rate their employer's support as poor or worse (23% vs. 18%), while Gen X employees (22%) were the most likely to give those lower ratings, followed by Gen Z (21%) and millennials (19%).
Many workers simply wanted clearer guidance. Over half of employees (52%) said they wished their employer communicated more clearly about ways to lower prescription costs.
For many companies, prescription affordability was already affecting the bottom line. Forty-two percent of healthcare decision-makers said prescription costs had been cited as a factor in an employee's decision to leave. Yet 26% said it was still not a current organizational priority.
Nearly half of healthcare decision-makers (47%) said their organizations have taken no steps to address prescription affordability. Only 30% said meaningful action is likely in the next 12 months, while 34% said it is unlikely.
Closing the Transparency Gap
This research makes clear that prescription affordability is not just a cost issue. It is an awareness, communication, and benefits design issue. When employees delay care, cut back on essentials, or search on their own for savings programs, the gap between available and usable support becomes impossible to ignore.
Closing that gap does not require an overhaul of benefits. It starts by embedding real-time prescription savings tools into existing member portals and benefit experiences without added friction. Buzz Health helps employers surface pricing options that make it easier for employees to choose lower-cost prescriptions, especially when coverage is limited or a medication isn’t fully covered.
Prescription discount cards, manufacturer copay programs, and state assistance resources already exist, but many employees don’t know how or when to use them. Buzz Health brings these options into a single, integrated experience, helping lower out-of-pocket costs, expand affordability beyond covered benefits, and support better adherence before costs become a barrier.
Methodology
We surveyed 1,007 full-time American employees to explore their experiences with prescription drug costs, awareness of affordability tools, and employer-provided benefits communication. The average age was 40; 51% of participants were female, and 48% were male. Generationally, 3% were baby boomers, 25% were Gen X, 57% were millennials, and 15% were Gen Z.
Additionally, we surveyed 250 healthcare decision-makers to assess how they perceive and address prescription drug affordability for the employees they serve. The average age was 41; 44% of participants were female, and 54% were male. Generationally, 6% were baby boomers, 22% were Gen X, 57% were millennials, and 15% were Gen Z.
About Buzz Health
Buzz Health is a healthcare technology company focused on improving medication affordability and transparency across the healthcare ecosystem. Founded 15 years ago as BuzzRx, a pharmacy discount card platform designed to help patients save on medications, the company has expanded to address upstream barriers in the prescription journey, including pricing complexity, coverage gaps, and disconnected systems. Today, BuzzRx remains a savings platform under the Buzz Health umbrella, while Buzz Health develops customizable technology that integrates with health systems to support the full prescription lifecycle and create a more transparent and cost-effective access model.
Fair Use Statement
This content may be shared for noncommercial purposes only with proper attribution to Buzz Health. When referencing or reposting these findings, please include a link back to Buzz Health.


